Pediatric Cardiology Testing
Testing may involve imaging of the heart (echocardiogram), evaluating the heart’s rhythm (electrocardiogram, ambulatory monitoring), examining the response of the heart and lungs to exercise (stress test, or exercise test), and evaluating risk factors for future heart health (blood pressure monitor, lipid panel). We also perform genetic testing related to the heart.
Read below to learn more about the different testing available through our clinic.
ECHOCARDIOGRAM
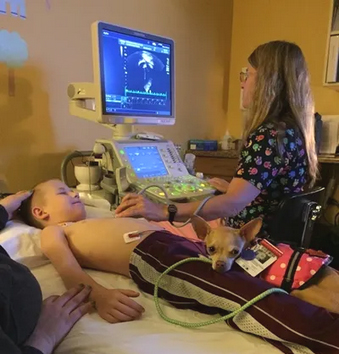
An echo is an ultrasound test used to evaluate the heart’s anatomy/blood vessels, blood flow, heart muscle function and pressures within the heart. It is similar to a “sonogram” during pregnancy.
+ What should I expect if my child needs an echo?
● Your child will be required to lie still and quiet on an exam bed for 30-60 minutes in order to obtain the highest quality images.
● SEDATION: For young patients or patients with developmental disabilities who are unable to cooperate, a light sedation medication may be required. Special “sedation instructions” will be provided prior to your appointment. Physician supervision is required for sedation, and therefore sedation will not be available for “echo only” visits.
● The echo room is darkened and equipped with a TV/DVD player and toys to occupy your child, and you may bring items that you think will assist your child in cooperating with the study. Examples include a pacifier, stuffed animal, or a favorite movie/TV show on an iPad or phone.
● The exam will be performed by a trained cardiac sonographer, who is registered in pediatric/congenital echocardiography.
● The upper body will need to be undressed. Gowns are available to maintain privacy.
● 3 electrodes (stickers) will be placed on the chest with wires attached to the ultrasound machine.
● The ultrasound transducer (camera/wand) with ultrasound gel will be placed in several different spots on the stomach, chest and neck to view the heart from different angles.
● The test is not painful but some light pressure will be applied to each of the camera positions.
EXERCISE STRESS TEST
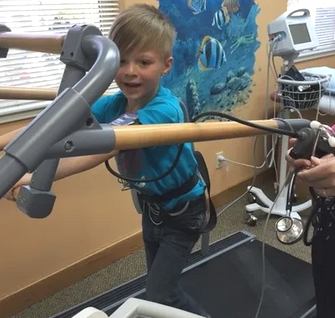
An exercise stress test is performed to assess the heart’s response to stress or exercise. The test is used to evaluate symptoms such as shortness of breath, lightheadedness, palpitations, and chest pain.
+What should I expect if my child needs a stress test?
● Your child should dress in comfortable exercise clothing and shoes.
● Electrodes and wires will be hooked up like an EKG (above).
● Your child will then walk on a treadmill starting slow and flat. The speed and incline will then be increased until a target heart rate is reached. As the speed of the treadmill increases, your child will need to jog, and then run. The exercise portion will typically last 5-20 minutes depending upon the fitness level of the child.
● Sometimes, especially if the test is being done in conjunction with PFT’s (pulmonary function testing, see below), your child will be running at an incline for the duration of the test, instead of gradually increasing the speed/incline.
● EKG’s will be printed periodically during the test, and blood pressure and heart rate will be recorded.
●In order to get the best information from the test, the child will be encouraged to continue for as long as they can, and to keep the technician informed of any symptoms they may be experiencing.
● When the target heart rate is reached, there will be a cool down period of slow walking followed by resting on an exam table.
● Your child will be watched for a few more minutes, as his/her heart rate comes down further. When finished, the wires and electrodes will be removed.
PULMONARY FUNCTION TEST
 A PFT is a test that determines how well your lungs work and diagnoses lung diseases. It will determine how much air your lungs can hold and how quickly you can move air in and out of your lungs.
A PFT is a test that determines how well your lungs work and diagnoses lung diseases. It will determine how much air your lungs can hold and how quickly you can move air in and out of your lungs.+What should I expect if my child needs a PFT?
● Your child will sit in a chair and be instructed to breathe in and out through a tube. The child will then be asked to take a deep breath and exhale as forcefully as possible through the tube. This will be repeated several times as the technician records the information in a computer.
● If PFT’s are performed in conjunction with an exercise (stress) test, your child will be asked to perform the test before exercise, and again several times after exercise.
● Sometimes, your child may be given an inhaler to see if this improves testing results.
Genetic Testing
ELECTROCARDIOGRAM (EKG)
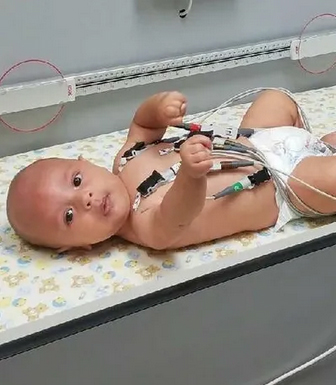
An EKG helps to identify heart rhythm abnormalities. It can also provide information about the size and thickness of the heart chambers and position of the heart within the chest.
+What should I expect if my child needs an EKG?
● Your child will be required to lie still on his/her back on an exam table for about 5 minutes.
● 10 small electrodes (stickers) will be placed on the chest and abdomen. Wires will be attached to connect the electrodes to the EKG machine.
● The technician will then print a paper copy of the electrical activity of the heart.
● The wires and electrodes will then be removed. Removal of the electrodes may feel like “taking off a bandaid.”
HOLTER MONITOR | ZIO PATCH

A Holter monitor is a longer (24 hours, or up to 2 weeks) recording of the electrical activity of the heart. It is used to detect irregularities such as bradycardia (slow rate), tachycardia (fast rate) and abnormal rhythms. Since irregularities can be intermittent, the continuous 1- to14-day recording has a greater chance of detecting abnormalities.
+What should I expect if my child needs a Holter monitor?
● Electrodes will be placed on your child’s chest (similar to an EKG above).
● Your child may participate in regularly scheduled activities except swimming.
● Your child will keep this attached for the designated time, then remove it when finished.
● You will then mail the monitor in the packaging supplied to you (or in some cases bring it back to the office) for interpretation.
● Your child may be asked to keep a log of symptoms during this period so that they can be correlated with the findings.
● In most cases, your child may shower while the monitor is attached.
AMBULATORY BLOOD PRESSURE MONITOR (ABPM)
 Ambulatory Blood Pressure Monitoring (ABPM) measures your blood pressure over the course of a full day (24 hours). You will wear a blood pressure cuff on your upper arm that is connected to a monitor. The monitor records your blood pressure readings both while you are awake and asleep.
Ambulatory Blood Pressure Monitoring (ABPM) measures your blood pressure over the course of a full day (24 hours). You will wear a blood pressure cuff on your upper arm that is connected to a monitor. The monitor records your blood pressure readings both while you are awake and asleep.
Why Monitor Blood Pressure for 24 hours? Measuring your blood pressure in your normal environment and during your usual daily routines gives your doctor a better idea of how your blood pressure changes throughout the day. Some reasons for having an ABPM:
● To determine whether medication is needed to treat your blood pressure.
● White coat hypertension: high blood pressure in clinic settings (around medical staff or doctors) with lower blood pressure outside of the clinic.
● Masked hypertension: blood pressure may be high throughout the day even if it is normal during your clinic visit.
● Nocturnal hypertension: high blood pressure at night can be indicative of other problems, such as sleep apnea.
● Hypertension medicine assessment: to make sure your blood pressure medicines are working as they should all day.
● Congenital heart disease: some heart defects, like coarctation of the aorta, are known to cause high blood pressure even after they are fixed.
The monitor is a small box that connects to the cuff on your arm. The monitor remains in a black pouch throughout the day. You may wear it with a belt to keep it up on your side and out of the way.
Important Reminders:
When the cuff inflates and you feel the cuff tightening, stop what you are doing and remain as still as possible (without putting yourself at risk). This allows the cuff to sense your blood pressure accurately. Relax your arm down by your side. If you are walking or standing, remain standing and drop the arm with the cuff to your side. If the monitor misses a reading, you will feel the cuff inflate again in 1-2 minutes to try another reading.
Recording Activities:
The activity log is an important part of the ABPM procedure. List changes in activity/symptoms throughout your day. If you are doing the same activity for an extended time, you do not need to write this over and over; instead, write ranges of time. Record your bedtime and wake time. Also record if you get up during the night to use the restroom or for any other reason.
Returning the Monitor:
The cuff, monitor, activity log, and belt (if you were given one) must be returned to the Children’s Heart Center. Follow the instructions given to you by the clinician. All ABPM equipment must be returned within 48 hours. Due to the expense of this equipment, it must be hand-delivered back; there is not a mail-back option. The monitor is a high value medical device and the patient is responsible for the cost of replacement if the monitor is not returned in a timely manner. This charge is not covered by insurance.
Results:
Upon return, a clinician will download the results from the monitor and prepare a report for the cardiologist. A final report will be sent to the provider who ordered the test, and that provider will give you the results. If you have not received a call within 1 week after returning the monitor, place a call to the provider who ordered the test to ask about the results.
If you have any questions or concerns while wearing the blood pressure monitor (ABPM), please call the Children’s Heart Center Monday through Friday between 8:00 AM and 5 PM at 541-639-8333.
Lipid Panels
Although our point of care lipid panels are an excellent screening tool, patients who have very high cholesterol levels, or those who need other blood tests in addition to their cholesterol, will still have their bloodwork done at a lab using a venous blood draw.

